What is vocal cord paralysis (Recurrent Laryngeal Nerve Paralysis)?
During breathing and producing voice, healthy vocal cords move with a physiological regularity. In patients with unilateral vocal cord paralysis, also called recurrent laryngeal nerve paralysis, the mobility of the paralyzed vocal fold is partially or completely impaired.
This disorder in vocal fold movement is usually caused by damage to the recurrent laryngeal nerve (RLN), the nerve which supplies the vocal cords and controls their physiological mobility.
Vocal cord paralysis can occur unilaterally or, in rare cases, bilaterally. The clinical picture of unilateral vocal cord paralysis, however, is highly distinctive from that of bilateral vocal cord paralysis.
The RLN, which supplies the vocal cords, takes a long winding course. Originating in the base of the skull, this nerve runs through the throat into the chest cavity and detours back up into the neck where it reaches the larynx.
The name derives from the fact that the recurrent laryngeal nerve curves back from the thoracic cavity into the laryngeal region (recurrere…[lat.] running back).
Vocal Cord Paralysis During Respiration
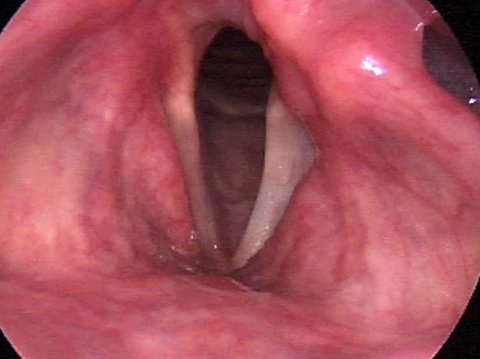

How does vocal cord paralysis develop?
There are many causes of unilateral vocal cord paralysis. The most common include:
- Thyroid surgery
- Surgery on the cervical spine
- Surgery on the carotid artery
- Tumors in the lungs
- Tumors of the bronchial tubes
- Other metastatic tumors
Vocal fold paralysis is also commonly diagnosed after protracted infections that later are presumed to have a viral pathogenesis.
If no direct culprit can be found responsible for the unilateral vocal fold paralysis, then this is called idiopathic. In such cases, it is imperative to do a comprehensive imaging study of the entire segment of the RLN. These scans are taken either by computed tomography (CT) or magnetic resonance imaging (MRI).
Paralyzed Vocal Cord During Phonation
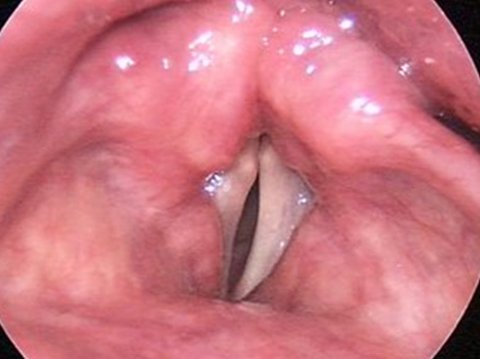

What symptoms are caused by vocal cord paralysis?
Recurrent Laryngeal Nerve paralysis can cause a variety of diverse symptoms. Nevertheless, the clinical picture is hallmarked by three major symptoms.
The most frequent symptoms of unilateral vocal cord paralysis are:
- Hoarseness
- Shortness of breath
- Swallowing difficulties
Patients with unilateral vocal cord paralysis primarily exhibit a more or less pronounced degree of hoarseness. Their voice is airy, veiled, and, in some cases, almost inaudible (aphonic).
The severity of hoarseness depends both on the position of the paralyzed vocal fold as well as on its degree of tension. If the gap between the vocal cords is small, the voice will be less breathy than when there is a large persistent gap.
Another very common symptom exhibited by patients with unilateral vocal cord paralysis is dyspnea — in other words, a subjectively perceived shortness of breath during speaking or physical exertion. This shortness of breath is not due to a lack of oxygen from insufficient ventilation, but to an excessive increase in the air consumed through the open glottis.
The patients are no longer capable of dosing air when speaking or producing voice; the air "evaporates“ and the patient has to gasp for air after a few words. The result is a manner of speaking that is constantly disturbed by interruptions in breathing. During physical exertion like climbing stairs, their inability to dose air also causes them to draw more air which is subjectively perceived as a shortness of breath or distressed respiration.
The third symptom regularly observed in patients with vocal cord paralysis is a frequent difficulty swallowing. In particular, these difficulties are manifest in the early phases of the paralysis. Patients will report that they have to be very careful when drinking carbonated beverages in order to avoid choking on the liquid.

What treatment options are available?
Unilateral vocal cord paralysis can be managed by two types of treatment:
- Voice therapy
- Phonosurgical therapy
If the Recurrent Laryngeal Nerve paralysis has emerged recently and diagnostics is completed, including exclusion of any malignant diseases, voice therapy ought to be initiated as soon as possible. This is important to foster the most rapid reactivation of the nerve and to counteract any atrophy that the vocal cord muscles may be experiencing. At the same time, the patient should be encouraged to speak normally, without falling into a dysfunctional pattern, in other words, not to speak with a pronounced whispering voice, for example.
Therefore, it is recommended that an intensive regimen of voice therapy be practiced two to three times a week. Voice rest or longer periods of silence should be avoided. In 80-90% of patients with vocal cord paralysis without evident injury to the RLN, complete recovery of the nerve can usually be achieved. Voice therapy can support the regeneration process.
Nevertheless, the nerve does not regenerate in around 10% of patients with idiopathic vocal cord paralysis. The voice then remains hoarse and the patient suffers from general impairment due to shortness of breath. Patients with irreversible intraoperative damage to the RLN are similarly affected by persistent hoarseness or shortness of breath.
A phonosurgical procedure can help these patients in an impressive manner. Today, several options are available for the surgical management of vocal cord paralysis.
The surgical method preferred by Dr. Wohlt is vocal fold augmentation. This procedure is described in detail in the section Voice Surgery for Vocal Cord Paralysis.
The results of this surgical method are so impressive because the procedure usually relieves the afflicted patients of these three hallmark and considerably burdensome symptoms: Firstly, the patients lose their hoarseness, the sound of their former voice is usually reinstated, their shortness of breath improves significantly, while their swallowing difficulties are likewise for the most part reduced.
Example of phonosurgical management of vocal cord paralysis
Vocal cord paralysis before surgery
Vocal cord paralysis after surgery

Truths and Myths About Vocal Cord Paralysis
Generally, the mobility of the paralyzed vocal fold can be expected to return within six months. Should voice therapy fail to bring back a satisfactory level of vocal quality, a phonosurgical intervention for reinstating voice function is usually recommended.
However, this time interval is not limited to six months. Indeed, patients would wait a year for their vocal fold mobility to return, although the probability decreases with increasing duration of the disease.
If the patient does not want to wait this long and chooses to undergo the surgery right away, this option is available at any time.
Although the fat augmentation will not reinstate mobility of the paralyzed vocal cord, the fat injected “upholsters” the tissue in such a way as to allow its healthy counterpart to medialize during voice production. That means the vocal folds can close again and the voice returns to its former, natural sound.
If the paralyzed vocal cord should later regain its dynamic ability to open and close, irrespective of whether it was operated on or not, the early augmentation procedure will not have had any disadvantages either, but will only have shortened the interval of voicelessness.

Case Report: Vocal Cord Paralysis
A 46-year-old elementary school teacher had undergone surgery for a suspected malignant disease of the thyroid gland. Immediately after surgery, she noticed a marked hoarseness in her voice. It was breathy, soft, almost inaudible. Even if she took great efforts, it was not possible for her to produce a resonant voice.
Moreover, she also sensed a marked shortness of breath. After speaking just a few words, she would have to gasp for breath and likewise had trouble during physical exertion. Moreover, she had a tendency to choke on liquids when drinking and had to cough often.
Recurrent Laryngeal Nerve paralysis had already been diagnosed during her postoperative hospital stay. She was discharged several days later and recommended to start a vocal exercise regimen with a voice therapist.
The videostroboscopic examination performed by the ENT specialist found immobility of the left vocal fold. Despite her greatest efforts, she was unable to close her vocal folds; a gap of 4–5 mm remained between them. Her voice was breathy to aphonic, with her average speaking pitch markedly raised.
The woman was initially advised to start an intensive regimen of voice exercises to be practiced three times a day. After four weeks at her follow-up exam, it was discovered that the mobility of her diseased vocal fold had improved. Over the further clinical course, voice therapy resulted in complete reinstatement of her vocal fold mobility. At two months’ follow-up, the patient reported that her vocal limitations had all disappeared. The quality of her voice was as good as before thyroid surgery, she no longer experienced any shortness of breath or swallowing difficulties.




